This study assessed the optimal plan for electrical field treatment, based on the positioning of an electrode array in patients with pancreatic cancer. Compared to the reference plan, the optimal plans generated by changing the position of the electrode array HELLO And Ci by 4.57% or 8.46%. In addition, it was found that the intensity of the electrical field within the tumor depends heavily on the position of the electrode array and is influenced by the position of organs and tumors in the body of every patient.
Since the pancreas is located near the center of the body, it was found that the electrode array of the reference plan are attached to the anterior posterior in the instructions of the anterior posterior and left to the right relative to the center of the tumor. Since the effectiveness of electrical field therapy is generally proportional to the intensity of the electrical field applied to the tumor [12, 13]The medium electrical field, minimal electrical field, HELLO And Ci Of the six test plans, those of the reference plan were compared. Generally higher average and minimal electric field and higher Ci indicate an electrical field with higher intensity in the tumor, which improves the efficiency of electrical field therapy. The fourth parameter, HELLOwas an indicator of the uniformity of the electrical field created in the tumor.
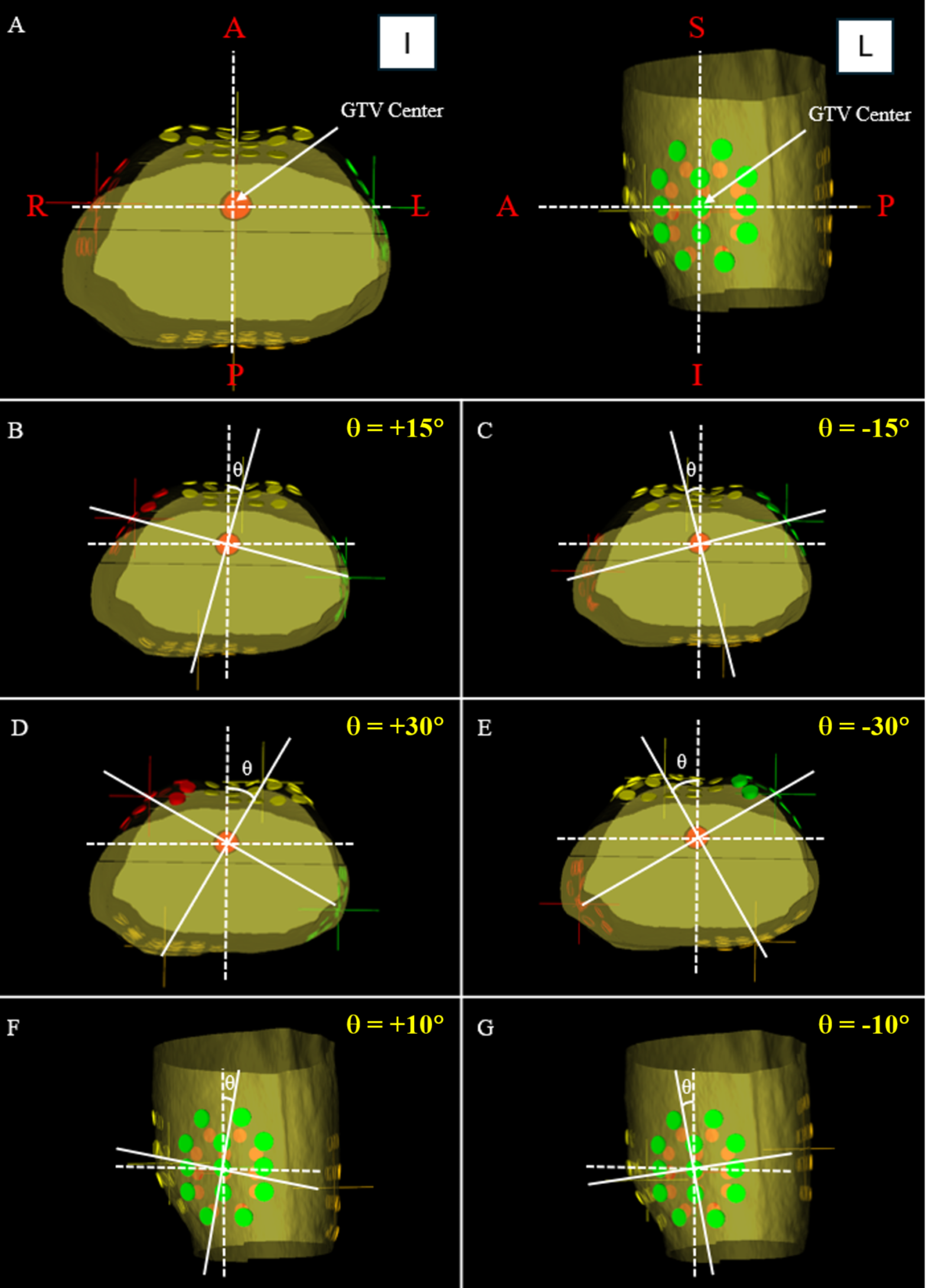
An earlier analysis of the effects of electrode positioning on the electrical field intensity in the treatment of brain cancer showed that depending on the position of the two electrode array pairs, the electrical field intensities of the optimized plan were∼17% higher than that of the reference plan [18]. Similarly, the present study showed that the optimized plan in which the position of the electrode array was changed by which in the reference plan was led to a higher electrical field in the tumor compared to the reference plan. The evaluation of the electrical field intensity within the tumor showed that the plans in which each electrode array was rotated in the axial level showed the highest electrical field intensities within the tumor for three or six patients. In contrast, the plan, in which each electrode array was rotated in the Sagittal level, resulted in the highest electrical field intensity within the tumor for the remaining four patients. Since the electrical field distribution of the location, shape and size of the tumor and the various organs is significantly influenced, it is difficult to predict the optimal location of the electrode array without actually calculating the electrical field distribution in the body of each patient with a 3D treatment planning system.
While electrical field therapy is generally well tolerated, it can cause certain side effects. Since adhesive electrode arrays have to be placed on the skin near the tumor position for treatment, most side effects are localized in these areas. One of the most commonly reported side effects is skin irritation and dermatitis, which can occur as reddening (erythema), rash, itching (pruritus) and in some cases bladder formation or ulcers. Since electrical field therapy has to wear patients for at least 18 ha days, a longer use can contribute to physical exhaustion over time. So far there is no strong indications that electrical field therapy causes organ oxicity, such as: However, it remains important to minimize the intensity of the electrical field in normal tissues, since excessive exposure may generate heat or damage the inner structures unintentionally.
The clinical implementation of electrical field therapy requires specialist knowledge of oncologists, medical physicists, nurses and device specialists to ensure proper treatment planning, verification and compliance with patients. Verification methods such as Array -placement monitoring, adherence tracking and evaluation of the skin condition play a crucial role in optimizing the treatment tax. However, variations of patient compliance, electrode positioning and tumor progression can lead to a distinction between the planned and the delivered treatment. Therefore, regular monitoring and support of the patients for maximizing the treatment effectiveness are of essential importance and at the same time the side effects. In addition, it is a crucial aspect of clinical implementation to ensure the exact submission of the intended electrical field during treatment. Yoon et al. Examination of a quality assurance system (QA) for electrical field therapy using a water phantom [19]. Your study showed that with 3D reviews the average differences in the voltage and in the electric field were 1.06% or 6.65%. These results are expected to improve the quality of electrical field therapy by providing experimental validation of electrical fields and improving predictions about the effectiveness of the treatment. However, further examinations are required to develop humanoid models in particular on inhomogeneous phantoms such as solid phantoms that could help to develop humanoids. These advanced models would enable more precise quality assurance (QA) and enable more precise simulation of realistic tissue diseases and further improvement in treatment accuracy.
While this study provides valuable insights into the effectiveness and feasibility of the treatment planning system for electrical field therapy, several restrictions must be recognized. First, the small sample size limits the ability to draw final conclusions and limit the statistical strength and generalizability. The expansion of the sample size into future studies will be of essential importance in order to improve statistical robustness, to improve the applicability of the results in different patient populations and to minimize potential distortions. Second, this study focuses on optimizing electrical positions based on the electrical field intensity in order to improve the effectiveness of treatment. However, an important restriction is the lack of direct clinical result data such as tumor response, patient survival or treatment -related side effects. While the optimization of electrode placement is essential for maximizing the field distribution, the actual therapeutic effects on patients still have to be validated by clinical research. Future studies should close this gap by combining computer optimization with the clinical result analysis in order to demonstrate the real advantages of optimized electrical field therapy. Thirdly, alternative optimization strategies such as conformic electrical field application or intensity -modulated electrical field application, which are based on voltage variations, optimize electrode positions based on the basis of electrical field intensity, but offer further improvements in treatment efficiency. These methods could enable more precise and patient-specific electrical field distributions and possibly improve tumor stargeting and at the same time minimize exposure to surrounding healthy tissues. Future studies should examine these advanced strategies in order to evaluate their feasibility, their therapeutic benefits and their clinical effects.
In addition, the effectiveness of electrical field therapy varies due to patient -specific factors, electrode positioning variations and anatomical changes during treatment. Differences in the electrical conductivity, the tissue density and the tumor composition influence the field distribution, whereby water -rich tissue (e.g. muscles, tumors) lead efficient fields as fat or bones. The variability of the tumor reaction and the sensitivity to skin further influences the treatment results. Personalized treatment planning and computer modeling can help optimize therapy for every patient. Regular surveillance and patient education are crucial for maintaining a consistent array positioning and adherence. In addition, anatomical changes during treatment such as tumor shrinkage, progression or weight fluctuations can change field distribution, while operations, radiation or fluid retention can further influence field penetration. Routine imaging and adaptive electrode placement are required to maintain optimal treatment output.
In summary, patient -specific factors, positioning accuracy and anatomical changes significantly influence electrical field therapy. Regular monitoring, imaging evaluations and treatment adjustments are important to maximize the effectiveness of the treatment and to improve the clinical results. Future studies should concentrate on the expansion of sample sizes, the integration of clinical result data and the investigation of advanced optimization techniques for further refining electrical field therapy and the improvement of real applicability.